Equine
Navicular Disease
By Lauren Lamb, DVM
Navicular ‘disease’ is a condition that affects the navicular bone, navicular bursa, deep digital flexor tendon and/or the associated ligaments attached to the navicular bone. Navicular disease, navicular syndrome, caudal heel pain syndrome in the horse, or insert some other name, are all terms used to describe the same condition, pain in the heel region of a horse. For the purposes of this article, navicular disease will be the term used to describe pain from the heel region of a horse. Navicular region will refer to the navicular bone, associated ligaments, navicular bursa and deep digital flexor tendon.
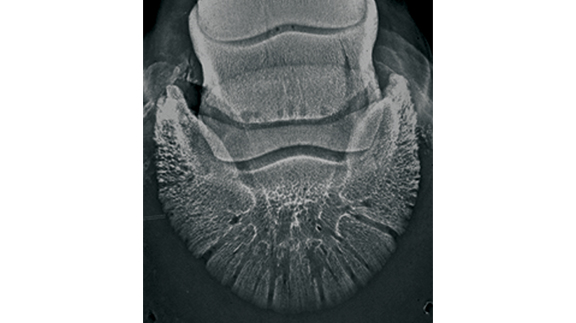
Before we can talk about navicular disease, we need to step back and review the normal anatomy. The navicular bone is located behind the coffin joint, within the hoof capsule. The navicular bone articulates (forms a joint) with the coffin bone and short pastern bone, which are located on the front side of the navicular bone.
The deep digital flexor tendon runs on the back side of the navicular bone. The navicular bursa lies between the navicular bone and the deep digital flexor tendon. The bursa is a fluid filled sac that functions as a shock absorber and a lubricant for the deep digital flexor as it passes around the navicular bone. Several other small ligaments help hold the navicular bone in place. These small ligaments are extremely important and frequently contribute to the horse’s pain.
The exact cause of navicular disease is unknown. Several potential causes for the disease have been proposed. Each theory revolves around some sort of trauma to the navicular bone and its associated ligaments, tendons or bursa. Another common theory is interference with the blood supply to the navicular bone. Navicular disease rarely develops in the hind limbs. It is predominantly seen in the front feet of a horse seven to 14 years of age. Thoroughbreds, Quarter Horses and Warmbloods are more commonly affected than other breeds. However, any breed of horse can develop navicular disease.
Lameness is the primary clinical sign seen in a horse with navicular disease. Navicular disease usually affects both front feet, but typically a horse will be more lame in the left or right leg. The lameness may only be seen with the leg on the inside of a small circle or when exercising on hard ground. The lameness will get worse with exercise and improve with rest. Typically Phenylbutazone (Bute) will improve the lameness to some degree.
Diagnosis can be challenging for a horse with navicular disease. The process of isolating the lameness to the heel region of a horse is easy and straight forward. This can be done with a temporary nerve block that will desensitize the horse’s heel. Once the lameness is localized to the heel, the real challenge of trying to identify the exact cause of heel pain begins.
Radiographs can be taken to evaluate the coffin joint, navicular bone and angles of the horse’s foot. The radiograph will provide little information regarding the soft tissue (ligaments and tendons) surrounding the navicular bone. Ultrasonography is typically used to image soft tissue structures in a horse; however, the location of the navicular bone within the hoof capsule makes ultrasound imaging challenging. The best way to image the navicular region is to use an MRI. The MRI provides the best quality imaging of both soft tissue and bone structures. The hoof wall does not influence the quality of image obtained with an MRI.
Pick up the June issue to learn more!
Equine
Equine Flexural Limb Deformities
By Dr. Garrett Metcalf
Flexural limb issues can occur in different age groups of horses, starting with newborns up to two- to three-year-olds. These issues occur somewhat predictably in age groups and can be addressed rather quickly when needed. There are various treatments and methods that can be used to address flexural issues. This article will discuss the most common flexural abnormalities and treatment methods.
Foal Flexural Issues
Foal flexural issues are often considered congenital flexural limb abnormalities because they are born with them. We don’t fully understand why this occurs but there is some evidence in the human literature that lack of fetal activity in the womb causes club feet in babies. In foals, it is thought that uterine positioning is to blame for part of the contracted tendons. Other causes can be exposure of the mare to toxic plants or substances that may be toxic to the fetus.
The most common area that a foal will have contracture of limb is at the carpus or knee. These foals will not be able to fully extend the knee and often will affect both at the same time. These foals can have difficulty standing to nurse or will get fatigued quickly and will not be able to stand for longer periods of time. There can also be damage to the extensor tendons or even rupture of extensor tendons caused by the high strain placed on them when the foal tries to stay standing. The rupturing of these tendons is not overly concerning but the lack of extensor function can make the flexural limb deformity worsen.
Other common locations of flexural limb deformities can be at the fetlock or coffin joint level. These deformities are not usually as detrimental to allowing the foal to stand and nurse properly compared to carpal flexural deformities. These deformities can be addressed similar to carpal deformities with some exceptions.
Treatment of Flexural Deformities
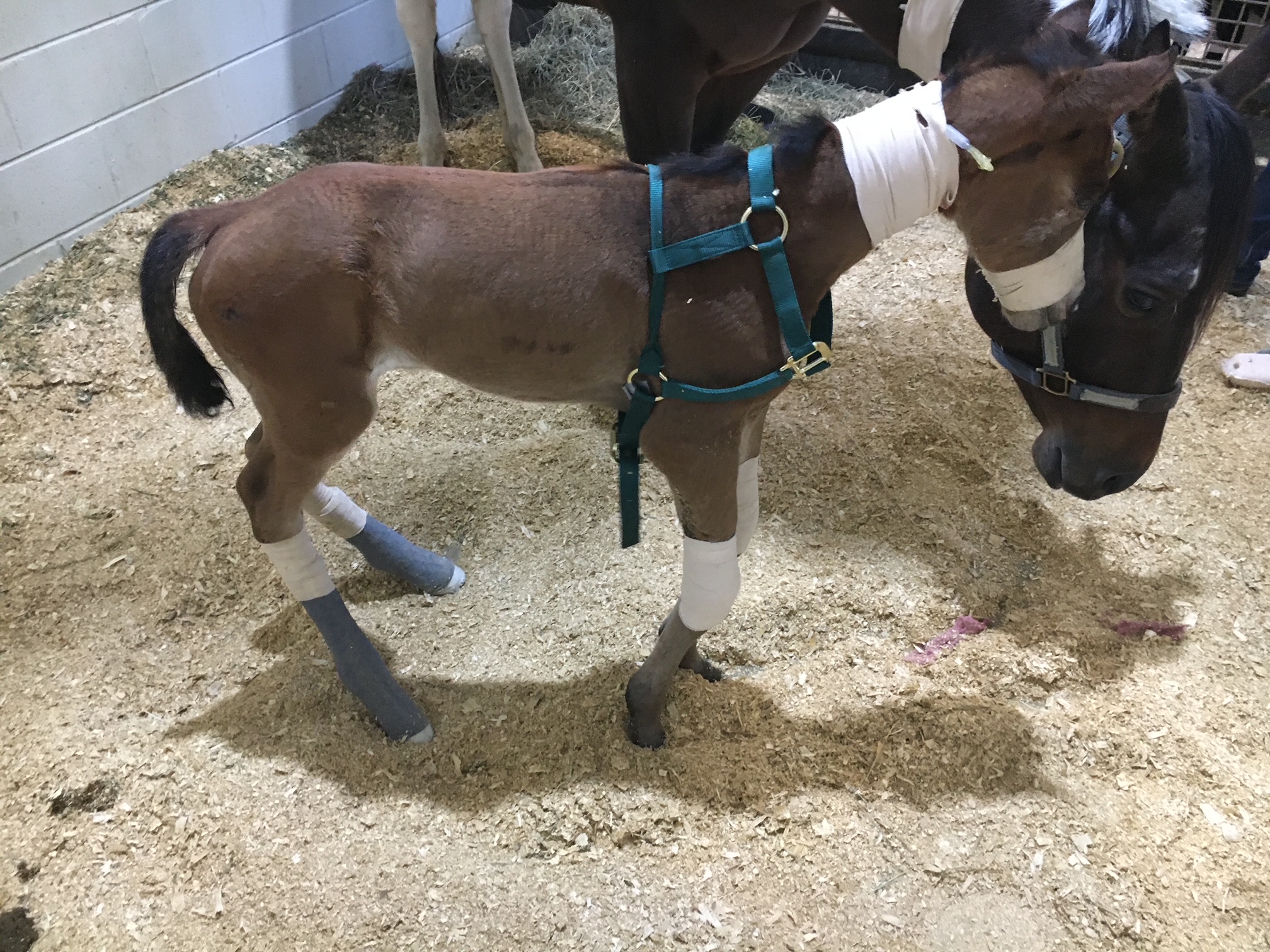
Splints or casts can be used to stretch and support the effected limbs of foals. Splints are often preferred by most veterinarians because they can be repositioned or reset as needed. Splints are easier to place on the limbs of foals but they do need resetting every 24 to 48 hours. Casting of the limbs is more rigid but is not adjustable once placed. Casting is often needed in more severe cases and requires changing frequently. Whenever placing these devices, care must be taken to prevent splint or cast sores because foal skin is rather delicate.
Surgical intervention is needed in some cases of carpal flexural deformities. A study out of Australia found that cutting of two muscle/tendon groups on the back of the carpus greatly improved the ability to extend the carpus with splinting methods. Cutting of these tendons do not have consequence to future athletic function. The two muscles are called flexor carpi ulnaris and ulnaris lateralis.
An antibiotic called Oxytetracycline is helpful to treat flexural limb deformities because of its side effect of causing tendon laxity. The laxity is created by chelating calcium within the tendons and allows the relaxation of tendons. This method does have some risk because of the high dose required and renal injury that it can cause when not administered with IV fluids.
Toe extension shoes are used when it comes to dealing with lower limb flexural limb deformities. These shoes are often applied with adhesives and after the splinting or casting is no longer needed. The toe extension shoe allow foal to continue to stretch those tendons every time they take a step and prevent from becoming contracted again.
Older horses (six months or older) with contracted tendons often get acquired limb deformities and the horses need surgical intervention to correct these deformities. These surgeries cut or release check ligaments that allows the musculotendinous unit of the deep digital or superficial digital flexor tendon to elongate. The deep digital flexor tendon is responsible for causing club feet or a flexural limb deformity at the coffin joint. The superficial digital flexor tendon is responsible flexor tendon that causes a flexural limb deformity at the fetlock joint. The check ligaments attach the tendon to bone and do not allow the tendon to elongate past a certain point. By eliminating these ligaments the flexural limb deformity can be corrected by allowing the muscle to stretch since the tendon is much more rigid.
Flexural limb deformities can be caused by excessive laxity or weakness of the tendons. These deformities are often seen in premature foals or foals that are born at a much smaller birth weight. The excessive laxity will cause the toes of there feet to flip up in the air and the fetlocks to be touching the ground. The areas where the skin is contacting the ground will cause sores and abrasions. If these areas are note protected the wounds can get into deep structures causing serious infection and injury the flexor tendons.
Treatment for tendon laxity is to add heel extension shoes to keep the toes flat to the ground. The extension behind the foot forces the toe down under the foals own weight. As the foal becomes stronger from normal activity the muscle attached to the tendons can support the foal and the limb laxity will correct itself. Abrasions still can occur even with heel extension shoes are in place so bandages need to be applied to protect these areas.
Flexural limb issues are a common issue that horses and owners will face. It is best to have your horse evaluated by a veterinarian whenever these problems are suspected. Foal flexural limb deformities can be life threatening because of the limitation of standing on time to nurse colostrum. Without colostrum within the first hours of life the foal is a much higher risk of sepsis and death.
Read more in the August 2023 issue of Oklahoma Farm & Ranch.
Equine
Equine Foot Abcesses

What a pain!
By Dr. Garrett Metcalf, DVM
A foot abscess is a common occurrence in horses throughout the year. Often wet weather can play a factor in the increase number of foot abscesses that horses will experience. A foot abscess can cause a great deal of pain, lameness, swelling and misery to the horse that often needs to be addressed quickly and provide pain management to keep them comfortable. There are many methods of addressing a foot abscess that people use. This article will discuss techniques to evaluate and treat the abscess as quickly as possible.
Foot abscess is a focal or sometimes diffuse infection that is trapped between the sensitive and non-sensitive lamina of the foot capsule. A foot abscess can form randomly from the normal stresses and environmental changes that cause the foot to allow bacteria to enter down to the sensitive tissues. Other causes are penetrating injuries to the bottom of the foot that allows bacteria to enter the through the outer lamina, such as nails, sharp rocks or even thorns. Poor foot care and misplaced shoeing nails can also lead to foot abscesses. A common area for abscesses to form is at the white line (area where the sole and hoof wall meet) and at the bars of the heels.
Foot abscess can cause a horse to have variable amounts of lameness, but generally they will be lame at a walk or even be non-weight bearing from the severity of the pain. Swelling starting at the foot and working its way up the limb can be noted when the abscess is trying to migrate out at the coronary band. These types of abscess are often referred to as “gravel” abscesses. “Gravel” is no more than just a regular foot abscess that has found the path of least resistance to the coronary band, where it ruptures out and causes a draining tract. An abscess in the hind foot can make the horse move rather abnormal to the point that it makes owners and veterinaries perceive the horse as acting neurologic.
Examination of the horse for lameness is the first step in diagnosing a foot abscess. The horse will often be lame at walk but some need to be watched at a trot to determine the lame limb. Lameness localization with regional nerve blocks can help make sure the pain is coming from the foot and not other parts of the limb. The foot will often have an increase digital pulse with occasional notable heat in the foot. The pulse is from inflammation causing a bounding of the digital arteries most notably behind the ankle region. The foot examination often needs to be performed with the shoe removed from the foot if the horse is shod. Hoof testers help pinpoint the area of most concern on the foot and often horses will be rather painful in response to the pressure created by the hoof testers. Knifing the foot out to clean up and remove any old sole or frog material is imperative to be able to locate the abscess with as much accuracy as possible. Often there will be a defect in the hoof or a dark focal tract that will lead to the abscess.
Treatment of the foot abscess can be done multiple ways and many people have lots of opinions on this topic. My treatment of choice is to open that abscess as soon as possible to give the horse nearly immediate relief and to quickly resolve the abscess infection. There are many methods to doing this but a good sharp hoof knife or loop knife one of the easiest ways to get the abscess drainage through the bottom of the foot. Whenever drainage of the abscess is achieved at the bottom this can eliminate the formation of a “gravel” and keep it from migrating out at the coronary band. Also drainage at the bottom allows a more effective treatment of the abscess with topically applied poultice agents. After the abscess has been opened to drain, bandaging the foot with a poultice agent is effective at eliminate the abscess and preventing foreign material from packing to the abscess area.
A great method of bandaging the foot is with the use of a large baby diaper. The diaper is very absorbent and foots the foot rather well. The diaper can be covered with layers of Vetrap, Duck Tape and Elaskiton to keep it protected or the foot can be placed in a medicine boot to keep the diaper protected.
Poultice choices are rather personal experience or availability, but also depend on the nature of the abscess. Epsom salt based foot poultice agent called Magna Paste or similar products are rather good at drawing out the remaining part of the abscess once it is opened. A homemade poultice of sugar combined with Betadine solution can make a really good poultice. There are various other topical agents that can be used effectively. The main thing when choosing a topical product is to make sure it is safe and that it has some antimicrobial properties.
Some foot abscess cases can be difficult to pinpoint and to drain. In these situations often time, pain management and soaking of the foot in Epsom salt water baths can help to allow the abscess rupture or make it easier to identify. In rather difficult abscess or when abscesses keep reoccurring in the same location, X-ray imaging of the foot is helpful to examine the structures of the foot. The abscess itself cannot be seen often with X-ray because the abscess fluid is the same density as the hoof wall. The only way to identify an abscess on X-ray is if there is gas present in the abscess making it visible on the film. Whenever there is a penetrating injury to the foot, X-ray is a must to make sure that the injury is not going into the deeper structures of the foot like the coffin joint or navicular bursa. These injuries are much more serious and need to be examined as quickly as possible. It is also recommended whenever possible to leave the penetrating object in the foot until the X-ray is taken. This will help the veterinarian understand what structures may have been injured.
Prevention of foot abscess is not always possible but a great start to this is really good hoof care. Routine trimming on a timely schedule is key part of good hoof care. The longer the feet go without a trim can affect the lamina and cause stretching of the white line, opening it up to allow bacteria to enter the foot. The use of special shoeing nails and other methods of good shoeing practices also limit the risk of abscessation.
Read more in the June issue of Oklahoma Farm & Ranch.
Equine
Guttural Pouch Diseases of Horses
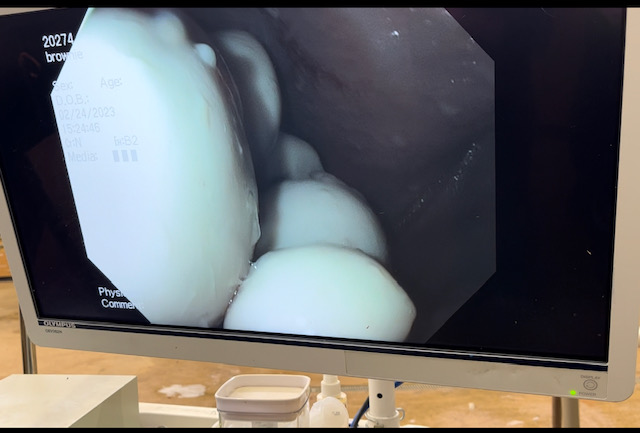
The guttural pouches of horses may not be very well known to most horse owners. These bilaterally paired pouches are located below the base of the skull, below the ears and extend into the throat latch region. The pouches purpose is not fully understood, but some theories is that they reduce the weight of the skull or have a blood cooling function to reduce the temperature of the arterial blood going to the brain. The guttural pouches can be plagued with a multitude of issues that are difficult to treat or can be life threatening to the horse. Other species contain guttural pouches such as some bats, American Forest mouse and Hyraxe.
The anatomy of the guttural pouches is complex and houses various important anatomic structures. The guttural pouches are an auditory tube diverticulum that is analogous to human Eustachian tubes but much larger. The volume of the guttural pouches can be up to 400-600 milliliters of air. The guttural pouches contain large arteries, nerves, the bones of the inner ear, muscle tissue and part of the hyoid apparatus that connects the skull to the larynx. The opening of the guttural pouches is deep in the nasopharynx through the slights call the pharyngeal ostium, which can only be accessed with an endoscope passed up the nose. The difficulty of accessing this area makes treatment of these diseases challenging at best. The guttural pouch is the only location in the horse that allows direct visualization of the arteries and nerves. The main arteries that are present in the guttural pouch are the maxillary artery and the internal and external carotid arteries that provide all the blood to the skull. The nerves in the guttural pouch are cranial nerves that exit directly from the brain or brain stem that innervate critical structures that control breathing, swallowing, chewing and ocular functions of the skull.
Read more in the April issue of Oklahoma Farm & Ranch.
-

 Country Lifestyle7 years ago
Country Lifestyle7 years agoJuly 2017 Profile: J.W. Hart
-

 Outdoors6 years ago
Outdoors6 years agoGrazing Oklahoma: Honey Locust
-

 Country Lifestyle2 years ago
Country Lifestyle2 years agoThe Two Sides of Colten Jesse
-

 Attractions7 years ago
Attractions7 years ago48 Hours in Atoka Remembered
-

 Farm & Ranch5 years ago
Farm & Ranch5 years agoHackberry (Celtis spp.)
-

 Outdoors4 years ago
Outdoors4 years agoPecan Production Information: Online Resources for Growers
-

 Equine6 years ago
Equine6 years agoUmbilical Hernia
-

 Country Lifestyle1 year ago
Country Lifestyle1 year agoSay Yes!











