Equine
Equine Laminitis – No Foot No Horse
Laminitis is probably by far the most devastating disease that a horse and horse owner will ever face. The definition of laminitis is nothing more than inflammation of the lamina or the tissue of the foot, but that does not describe the devastating pain and struggle that a horse faces with this disease. There are many sources of laminitis or foundering in horses. I will cover some of the most common causes, ways to avoid these causes and treatments.
The foot is an amazing organ for the horse and it is amazingly resilient but at the same time very fragile. The equid foot has to endure nearly constant loads of just daily locomotion but also endure very high levels of load during events such as racing, jumping and pulling. The tissue that holds the foot attached to the coffin bone is only a few millimeters thick but is amazingly strong. The tissue looks like Velcro under a microscope and is very rigid but also at the same time allows the foot to flex, grow and expand. The metabolic energy and blood flow rate that feet require to with stand this load is incredibly high as well. The blood flow to the very farthest part of the horse is complex and important when addressing laminitis which will be discussed later.
Causes –
- Grain overload or carbohydrate overload
Consumption of a large amount of grain can lead to gastrointestinal disruption leading to founder. A horse that breaks into the feed shed and consumes large amounts is the most common scenario that is seen. These horses need to have as much grain removed from their stomach as soon as possible with a stomach tube and then products such as activated charcoal administered to help bind toxins that may be produced from bacteria dying off from the high grain load in the gut.
- Metabolic conditions – PPID (Cushings) and EMS (Equine Metabolic Syndrome)
Horses with cushings have high levels of glucocorticoids circulating in their blood leading to disruptions of the lamina along with other body systems. These abnormally high glucocorticoids are caused by an abnormality with the pituitary gland in the brain. This can be corrected when diagnosed with medication.
The EMS horses have high levels of insulin which has been found experimentally to induce laminitis. Horses that are obese and get very little exercise are at risk of EMS. EMS is reversible and prevented by managing diet more closely, routine exercise and preventing access to lush green pastures.
- Lush green grass (Grass Founder) – commonly seen in overweight EMS horses
Similarly, horses with underling EMS can found on lush green growing grass because of the high sugar content in these grasses. In the spring with good grains and plenty of sunshine grass can grow rapidly. This rapid growth phase of grass produces larger amounts of sugars in the blades of the grass during photosynthesis. It has been discovered that during peak sunlight is when the highest sugar content is found in the grass because of higher amounts of photosynthesis occurring in the grass blades.
- Endotoxemia – Caused by severe illness such as sepsis, colic, pneumonia
Horses that have serious bacterial infections or acute colitis can absorb endotoxins released by the dead bacteria. Horses are extremely sensitive to endotoxins and these toxins are called LPS (lipopolysaccharides) that make up part of the bacteria cell wall. When a large amount bacteria are killed off with antibiotics or disruptions in the horses gut these toxins are absorbed causing lots of problems for the horse.
- Overloading weight – injuries that cause the horse to bear more weight on another limb
Overbearing weight on other limbs from an injury to another limb can cause contralateral limb laminitis. Just by shear overloading force breaks down another foot. This can occur when a major injury occurs to a limb forcing more weight onto another because of pain. This is seen commonly with fractures, serious soft tissue injuries and neurologic conditions. This is what led to the death of Barbaro, the famous thoroughbred race horse that fractured his leg during the Preakness.
- Black Walnut – Shavings containing black walnut can induce laminitis
The species of tree can be very toxic to horses and must never be used as bedding or shavings that will come in contact with horses. It has been estimated that shavings containing as little as 5% black walnut can be toxin to horses. Some research has even thought that contact along can be deadly.
Diagnosing laminitis is rather straight forward. Examination of the horses gait at a walk or trot will indicate lameness. Most horses in acute founder will be severely lame at a walk and will be shifting weight back to the hind limbs in order to move or change directions when ask to ambulate. Horses will have an increased pulse in the arteries near the feet called a digital pulse. This pulsation of blood is similar to the throbbing sensation that we feel have an acute injury to a finger or limb and is quit notable in acute laminitis. Heat can also be noted around the coronary bands and hoof wall.
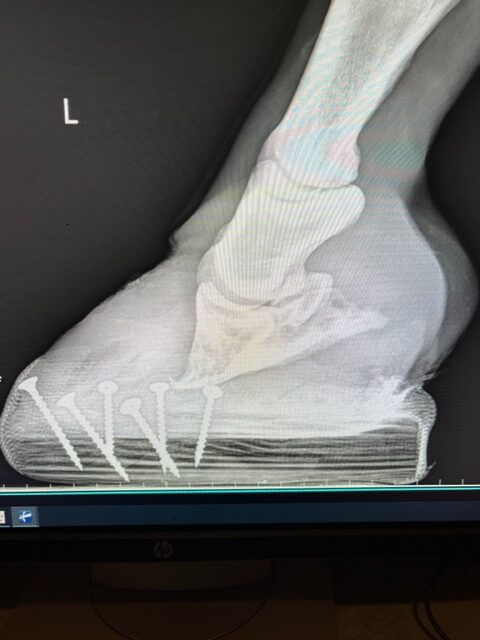
Radiographs or x-rays are used determine the severity of laminitis by measuring the separation of the coffin bone from the hoof wall. Venograms are also used to identify the blood flow damage to the foot using contrast dies injected into the digital veins while a tourniquet is applied above the foot. The contrast highlights the blood vessels so they can be seen with x-ray.
Treatment of Laminitis
First of the underlying cause of the laminitis must be eliminated or managed in order to get the laminitis under control or the battle will be very difficult. For example if a horse with EMS is not put on a serious diet and their weight managed you will be fighting a losing battle. Secondly a veterinarian and a farrier team are going to be needed to help manage the horse’s feet to prevent further laminar damage and provide the best possible foot support needed. Veterinarians must provide pain management, systemic care or treatment of the underlying illness and administer other medications that can benefit the horse in order to eliminate laminitis. Farrier’s have the daunting task of providing support of 1,000 pound or more horse that has feet sometimes the size of tea cups. The goal for farriers is to provide the proper support with various different methods across the sole of the foot at the same time eliminating stress and forces that inherently designed into the horse’s foot. Care for the horse’s feet is very critical and requires a skilled team to provide the best care. Lastly is that you have to be in it to win it. Short cuts and half hearted attempts are usually not very fruitful when it comes to dealing with laminitis. Below is a list of treatments used to treat laminitis.
- Medication or surgery to correct the underlying cause
- Cryotherapy or icing of the lower limbs and feet
- Systemic anti-inflammatory drugs and pain management
- General health care such as a good diet, deep beading, management of other illnesses and supportive care
- Corrective foot care
- Surgical intervention with tenotomies (cutting the deep digital flexor tendon)
- Slings (rarely available and only in extreme cases)
Laminitis or founder can be very challenging to correct or manage. It is not uncommon to humanely euthanize horses for acute or chronic causes of founder. These horses are often losing weight, unable to get up and ambulate well enough to eat or drink frequently enough. Often it is important to have a discussion of quality of life on behalf of the horse and do what is necessary so the horse is not suffering. These are always difficult decisions but they are necessary and always good to have these with your veterinarian and farrier that are caring for the horse.
Read more about your horse’s health in the latest issue of Oklahoma Farm & Ranch magazine.
Equine
Degenerative Suspensory Ligament Desmitis of the Horse
By Dr. Garrett Metcalf
The suspensory ligament is a vital component of the limb of a horse to produce normal locomotion and support. The suspensory ligament is a common area of concern in performance horses of various disciplines and can be single handedly the cause of lameness or performance issues. This article is going to look at a specific degenerative disease of the suspensory ligament and what horses are at risk for this disease.
DSLD or degenerative suspensory ligament desmitis was first discovered in the early 1980’s in Peruvian Paso horses. The name has been changed because the suspensory ligament is not the only organ affected from the disease but the suspensory is ultimately the biggest issue. The newer name, ESPA or equine systemic proteoglycan accumulation, is more correct because other ligaments and tissues are affected by this disease. In this article we will only focus on the suspensory ligament. The most commonly affected breeds are Peruvian Paso, Paso Fino, Morgan, Saddlebred, Warmblood, Paints, American Quarter Horse, and Thoroughbred breeds. The age of onset of the disease is variable among breeds but it is more common to be seen in middle age to older horses. However it has been documented in horses as young as one year of age. The disease generally will have a slow insidious onset that can go undiagnosed for months or years depending on the horses work and discipline.
A horse that begins to show early signs of DSLD may have a vague lameness issue that is difficult to isolate and they most likely will resolve with a period of rest. As the horse returns to moderate level of work the lameness will return. This scenario may go on for several months or more before the discovery of the DSLD is made. The first indication of DSLD is often pain isolated in the suspensory branches or fetlock region when a flexion test is performed. Horses with DSLD will also have a “dropped” fetlock appearance because the suspensory is the main supporting structure of the fetlock joint. DSLD can affect the hind limbs, forelimbs or all limbs at the same time. A unique sign of DSLD is that not just one limb is affected but rather bilaterally affecting the limbs, meaning it will either affect either both forelimbs or hind limbs at the same time. It is my experience that the hind limbs are more commonly affected compared to the forelimbs. Horses will often have enlargement of the fetlock region and increased joint fluid or wind puffs. Horses will often have a straight hock or post legged hind limb appearance. Horses will often shift weight frequently in an effort to get relief from the discomfort and this can be confused with other lameness issues or foot related pain.
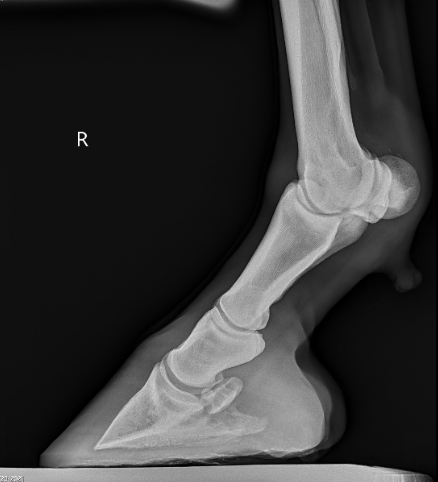
Diagnosis of DSLD is often made by clinical signs, breed and ultrasound findings. Ultrasound imaging of the suspensory ligaments will often show diffuse enlargement of the suspensory body and branches. The suspensory ligament will have a poor heterogeneous fiber pattern with periligamentious soft issue thickening from scar tissue deposition and edema or fluid within the tissue. Radiographs of the lower limb may reveal abnormal bone changes in the sesamoid bones behind the fetlock joints and even osteoarthritis of the pastern and or fetlock joints. A definitive diagnosis can be made from a biopsy of a ligament in the neck called the nuchal ligament, but is not often performed because of the invasiveness of the biopsy.
Treatment is very limited and it is mostly geared towards protection of further damage by prolonged rest. Pain management is also important to attempt to keep the horse as comfortable as possible. Different shoeing techniques can be used with marginal success. In early cases of DSLD, a suspensory shoe that helps engage more work from the deep digital flexor tendon can help elevate the fetlock and offer more protection to the suspensory ligament. The devastating thing about this disease is that there is no cure and there are hardly any good options to slow the progression of the disease. DSLD carries a poor prognosis when the diagnosis is made in any breed of horse or any discipline. Although some cases can be managed better than others, it often progresses to the point of debilitating pain and discomfort to the point of humane euthanasia especially in the Peruvian Paso breed.
Read more in the February 2023 issue of Oklahoma Farm & Ranch.
Equine
Gastric Ulcers

By Dr. Devan England DVM
Does your horse have gastric ulcers? Gastric or stomach ulcers are frequently blamed for a variety of things including poor performance, acting ‘cinchy’, weight loss, not eating, poor coat condition, diarrhea and colic. However, gastric ulcers are not always the culprit and the only way to know for sure if your horse has gastric ulcers is to look at the stomach on camera, using an endoscope. Poor appetite and poor body condition are the mostly widely observed clinical signs with gastric ulcers, however, these are non-specific. If you think your horse might have gastric ulcers, the best place to start is to talk to your veterinarian and consider scheduling a gastroscopy. Gastroscopy requires the horse be held off feed for at least 16-18 hours and held off water for at least 6-8 hours. Fasting off feed and water is necessary to allow the veterinarian to see the whole stomach. If restricting feed or water is difficult in your management situation, many veterinarians will allow you to hospitalize your horse the night before gastroscopy for proper fasting.
Gastric ulcers are split into two types, classified by the location of the ulcer in the stomach. Squamous ulcers are ulcers that occur in the squamous or skin like portion of the stomach. This is the top part of the horse’s stomach, is closest to the esophagus, and has squamous tissue to protect this portion of the stomach from stomach acids. The other ulcer type are glandular ulcers. Glandular ulcers occur in the bottom portion of the stomach, which is closest to the small intestine. This portion of the stomach has glandular mucosa with cells responsible for producing stomach acids for digestion as well as cells that produce mucus and buffers to protect the lining from stomach acid. Gastroscopy is important not only for diagnosing whether ulcers are present but also determining the severity and the type of ulcer, because these two ulcer types require different treatments.
Squamous gastric ulcers are common in racehorses both in and out of training, with higher prevalence in racehorses under training. Prevalence in Thoroughbred racehorses in training has been reported to be up to 100% (Sykes 2015). Squamous ulcers are also prevalent in Western pleasure horses, Thoroughbred stallions on breeding farms, and Italian donkeys (Sykes 2015). Glandular gastric ulcer prevalence has not been as well described as squamous ulcers. Glandular ulcers are reported to be most common in Thoroughbred and Standardbred racehorses, Canadian showjumpers and polo ponies, and American Quarter Horses (Sykes 2015).
Risk factors for ulcers vary by ulcer type. Anti-inflammatories (Bute, Banamine) can increase the risk of glandular ulcers in some horses by affecting normal defense mechanisms but are not a high risk in most horses. Horses that display stereotypic behaviors, such as cribbing, have an increased risk of squamous ulcers. Grain fed before hay in non-exercising horses, feeding larger amounts of grain, and increased time between meals increases the risk of squamous ulcers. Increased time with high intensity exercise and housing in single pens is associated with increased risk of glandular ulcers. A straw only diet, lack of water access and lack of direct contact with other horses increases the general risk of gastric ulcers.
If your horse is diagnosed with ulcers, the mainstay of treatment is a buffered formulation of omeprazole (Gastrogard, Ulcergard). Over the counter Omeprazole and compounded Omeprazole are not effective because without buffering, the acidic stomach quickly breaks down the drug before absorption. Most horses with squamous ulcers will have healing of these ulcers after a 4-week course of Gastrogard or Ulcergard at treatment dose (whole tube for the average horse). Some horses may be healed by 3 weeks of treatment, but all horses should undergo a recheck gastroscopy before stopping treatment. Horses diagnosed with glandular ulcers need combination therapy with Gastrogard/Ulcergard and Sucralfate for 4 weeks. About 2/3 of horses with glandular ulcers will heal in this time, but some horses may require longer treatment times so a recheck is always recommended before discontinuing treatment.
Horses at higher risk of gastric ulcers may benefit from preventative (low) doses of Ulcergard (1/4 tube in average sized horse) given for a few days before and during high stress situations like long distance travel and competitions. Sea buckthorn berry supplement may be protective against formation of glandular ulcers. Dietary management to decrease the risk of ulcers includes providing more frequent small hay meals if pasture access is not available, limiting high sugar grains as much as possible and adding vegetable oil to the feed.
Sykes BW, Hewetson M, Hepburn RJ, Luthersson N, Tamzali Y. European college of equine internal medicine consensus statement – equine gastric ulcer syndrome in adult horses. J Vet Internal Med 2015; 29:1288-1299.
Equine
Trailer Safety Checklist

By Janis Blackwell
As the season arrives to gear up for participation in your equine event of choice, one thing remains a constant for all horse owners. That constant is our responsibility to insure the safety of our horses by being diligent to maintain the integrity of the trailers in which we haul them. There are a number of things that can be dangerous both inside and outside of your trailer. Whether you traveled all winter long or whether your trailer sat unused or was used very little through the cold weather months, at least once a year your trailer is due a thorough going over. So here we go with a checklist that will help you insure a happy and safe trip for you and your equine partner.
- A sound floor is absolutely imperative. Whether your floor is aluminum, steel or wood, it should be cleaned regularly after use to preserve it. Urine and manure will erode and weaken all types of floors. Even rubber mats will not prevent erosion of your floor. (Maintenance tip: remove mats and wash aluminum floors often to prevent erosion.)
- Especially check wooden floors for rotten boards. Immediately replace questionable flooring before hauling. (Maintenance tip: For wood, remove mats and wash out manure and debris. Coat wooden floor in a cheap motor oil. Allow to sit in hot summer weather until the oil soaks in. Be careful—floor will be slippery until oil cures into the wood. This treatment yearly will preserve a wooden floor for much longer than normal as it repels urine and protects the wood).
- Keep the interior and exterior washed to enable you to check for rusted out places, leaks, etc.
- Have a professional check your brakes at least once yearly to be sure they are operating properly.
- Be sure tires are inflated to the proper air pressure, and check the inside of each tire for hidden unusual wear that could cause a blowout. Replace worn tires before leaving home.
- Wheel bearings must be checked and packed at least once a year. This should be done even if the trailer has been rarely used since the last time the wheel bearings were packed. In fact, trailer maintenance professionals say that sitting stationary and unused is even worse for the bearings. Improper care and maintenance of wheel bearings can cause a wheel to seize up and actually twist off while in use. Use a horse trailer professional for this maintenance task.
- Axles should be checked for bowing. A bent or bowed axle can cause excessive tire wear and damage wheel bearings.
- There should be no more than two inches in height difference from the front of the trailer to the back. More difference than that causes the bulk of weight of the trailer and its contents to ride mostly on the rear axle causing it to bow and wear on both tires and wheel bearings.
- Another critical part of the trailer to keep an eye on are the butt chain or bar and the back door. The butt chain or bar should be firmly attached to the wall and its keeper and should always be latched. The door should have a strong secure latch with a pin to insure it stays latched while in motion.
- Finally, but certainly not of least importance is a thorough check of the trailer hitch including ball and coupling. Keep the ball well greased. Periodically, check to see that the ball is still securely tightened and the latch on the coupling is working properly.
These few critical safety check points can save you money, stress and the wellbeing of your horse. Until next time, happy trails and safe traveling.
This article was originally published in the April 2016 issue of Oklahoma Farm & Ranch.
-

 Country Lifestyle2 years ago
Country Lifestyle2 years agoJuly 2017 Profile: J.W. Hart
-

 Attractions9 years ago
Attractions9 years ago48 Hours in Atoka Remembered
-

 Equine9 years ago
Equine9 years agoUmbilical Hernia
-

 Outdoors8 years ago
Outdoors8 years agoGrazing Oklahoma: Honey Locust
-

 Country Lifestyle4 years ago
Country Lifestyle4 years agoThe Two Sides of Colten Jesse
-

 Farm & Ranch1 year ago
Farm & Ranch1 year agoFrom Plow to Plentiful: The Most Important Inventions in Agricultural History
-

 Farm & Ranch8 years ago
Farm & Ranch8 years agoHackberry (Celtis spp.)
-

 Equine6 years ago
Equine6 years agoOn the Road with Emily Miller-Beisel





